
Jul 14, 2020 | Postpartum
Let’s Talk About It
The pelvic floor often gets ignored during regular checkups in postpartum, but are vital to our sexual and reproductive health. I talked about pelvic floor muscles during pregnancy in my previous blog post and now it’s time to talk about some of the nitty gritty details of pelvic health and postpartum. While our bodies expand and change in beautiful and often uncomfortable ways during pregnancy, they also go through A LOT during labor and birth. Our perineum has to stretch during vaginal birth and that, along with tearing, can have an impact on your pelvic floor health in postpartum and beyond.
Many new moms experience pelvic floor issues after vaginal birth and don’t seek treatment because women’s health is often stigmatized. So let’s talk about it! It’s the only way to push back and normalize the experiences of birthing people.
Once again, I reached out to Dr. Rachel Parrotta, DPT, for her take.
What’s Normal

Certain exercises like this bridge can help strengthen core and pelvic muscles
“The pelvic floor muscles undergo a very large stretch during vaginal birth and the pelvic region can be quite swollen in the first few weeks post-partum,” said Dr. Parrotta. “These factors can make it very challenging to coordinate your pelvic floor muscles (aka ‘Find your Kegel’) in the first few weeks after birth. Learning and practicing pelvic floor muscle coordination prior to birth can help develop ‘muscle memory’ that will assist you in postpartum recovery.”
I have oft heard phrases like “birth will wreck your vagina” said to new moms and it’s untrue. As Dr. Parrotta mentioned, the vagina and pelvic muscles largely expand. But, here’s the thing – they are meant to do this. After vaginal birth, your pelvic floor is bound to be swollen and aggravated. So, it’s completely normal to experience some postpartum incontinence and perineal discomfort in the following weeks.
What’s Not Normal
If you experience any of the following after you’re six-weeks pospartum, visit your care provider and seek out a pelvic health specialist:
- Pain during sex
- Perineal pain
- A heavy feeling or pressure in your perineal area
- Incontinence
- Difficulty urinating or passing a soft bowel movement
Final Thought
Your pelvic health is important. A healthy pelvic floor after postpartum can lead to better sexual satisfaction for you, more stability in your pelvic region, and better outcomes in future pregnancies.
Pelvic PT can be intimate, but it shouldn’t feel invasive. Find a practitioner you trust and get evaluated, because your health is worth it.

Jul 2, 2020 | Birth
Pelvic What?
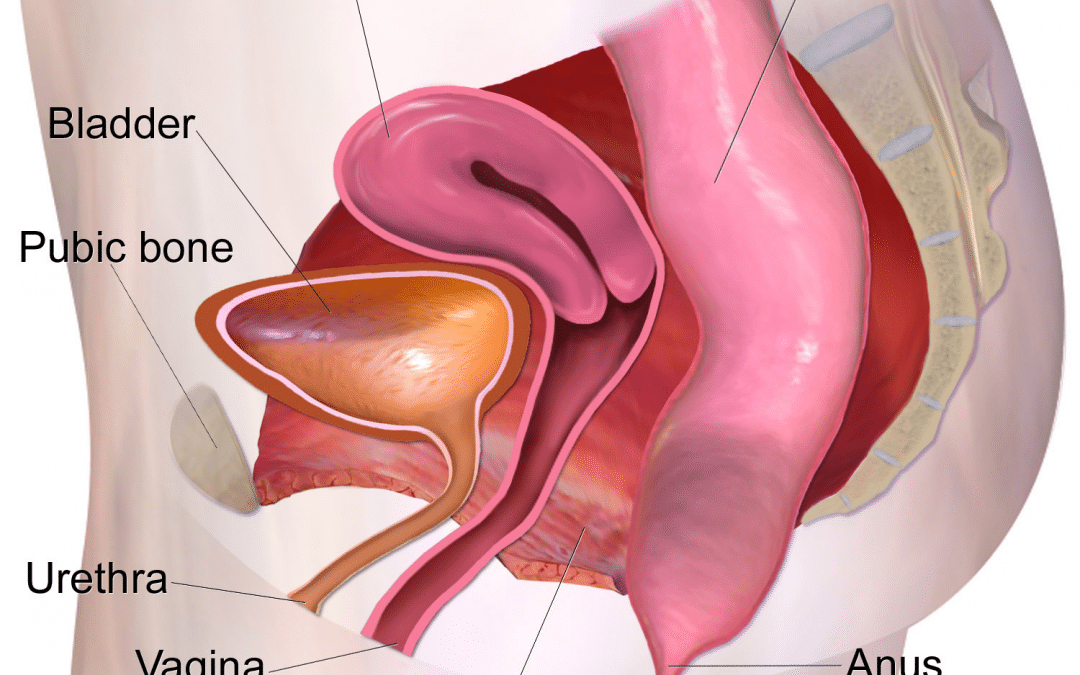
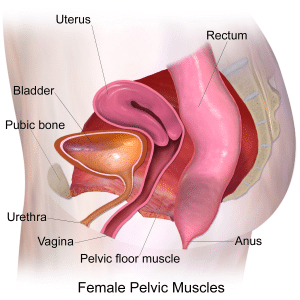
 The pelvic floor is the layer of muscles that stretch under the pelvis and support the inner organs (bowels, uterus, and bladder). I had never heard of the pelvic floor until I started learning about pregnancy and birth. Even though I was already suffering from and getting treated for a pelvic floor dysfunction long before I became pregnant, no one, not my OB or physical therapist, explained what the pelvic floor muscles did and how they could impact my well-being.
The pelvic floor is the layer of muscles that stretch under the pelvis and support the inner organs (bowels, uterus, and bladder). I had never heard of the pelvic floor until I started learning about pregnancy and birth. Even though I was already suffering from and getting treated for a pelvic floor dysfunction long before I became pregnant, no one, not my OB or physical therapist, explained what the pelvic floor muscles did and how they could impact my well-being.
Turns out, as I would later learn, my pelvic floor could wreak a lot of havoc on my body during pregnancy and labor. My pelvic instability lead to symphysis pubis disorder that caused excruciating pelvic girdle pain that still lingers today, one year after I gave birth. The pulling on my pelvic muscles also lead to a lot of back pain.
To learn more about pelvic health, I reached out to Rachel Parrotta, DPT, a pelvic health physical therapist.
During Birth
“I believe that all people would benefit from learning about their pelvic floor muscles prior to giving birth,” Dr. Parrotta said. “Since we are often unfamiliar with these muscles, it can be difficult for people to use their pelvic floor muscles in ways that help facilitate both birthing and post-partum recovery.”
Imagine, you are in labor and your care provider says, “Okay, it’s time to push.” Many birthing people may feel that bearing down feeling, that urgent need and desire to push. However, receiving an epidural can prevent people from experiencing bearing down and even from pushing effectively because the abdominal and pelvic floor muscles feel numb. Care providers do something called “coached” or “directed pushing” until the laboring person gets the hang of how to push. Your care provider will tell you when and how to push in accordance with your contractions.
This happened to me. I got an epidural during back labor and didn’t have the bear down feeling until my water broke. My midwife coached my pushing because I wasn’t using my pelvic floor muscles correctly. She told me I wasn’t doing right. She got frustrated and impatient with me. She actually shoved her finger up my bum WITHOUT INFORMED CONSENT to pinpoint the muscles I should be using – an action that still makes me shudder and feel small to this day. I don’t want this to happen to you.
Pushing Practice
Ideally, we want our pelvic floor muscles to be relaxed during the second stage of labor (pushing), as tensing those muscles can actually delay birth. You can go to a professional like Dr. Parrotta to identify your pelvic floor muscles and learn how to use them for pushing BEFORE labor.
“Learning about your pelvic floor muscles prior to birth can help prepare for a more effective pushing phase of birth, especially if a person is planning on birthing with an obstetrician and/or with an epidural,” said Dr. Parrotta.
Pushing your baby into the world is a powerful action that we are all capable of doing. Exploring your pelvic floor to ensure its health and learn about its abilities can make an impact on your birth and postpartum experiences.

Mar 13, 2020 | Birth, Postpartum
Tensions about COVID-19, a type of coronavirus, are rising in the United States as the illness has been spreading. Travel is becoming restricted, people are working from home, schools are closing, and apparently toilet paper is now a hot commodity. Many are starting to panic. The symptoms of COVID-19 have mainly proven to be more serious in older patients and those with serious complications such as heart and lung disease, and diabetes. But what about pregnant women and new moms?
Are Pregnant Women More Susceptible to Getting COVID-19 or at Higher Risk of Serious Illness?
At this time, the CDC does not have conclusive information. However, the physiological changes women experience during pregnancy do tend to make them more susceptible to viral respiratory infections. The CDC advises pregnant women to take standard precautions like washing their hands and avoiding other people who are sick.
Can COVID-19 be Transmitted to Babies During Pregnancy or Vaginal Birth?
The virus is currently thought to only be spread through respiratory droplets, meaning through fluids expelled by the mouth and nose during coughs, sneezes or intimate contact. It is unknown if the virus can be transmitted through the womb. However, the CDC said, “In limited recent case series of infants born to mothers with COVID-19 published in the peer-reviewed literature, none of the infants have tested positive for the virus that causes COVID-19. Additionally, virus was not detected in samples of amniotic fluid or breastmilk.”
Can I Continue Breastfeeding?
 So far, no evidence of the virus has been found in breast milk. La Leche League International (LLLI) advises women to continue breastfeeding unless a care provider deems it medically necessary to stop. Human milk provides important immunological antibodies produced in the mothers body to the baby.
So far, no evidence of the virus has been found in breast milk. La Leche League International (LLLI) advises women to continue breastfeeding unless a care provider deems it medically necessary to stop. Human milk provides important immunological antibodies produced in the mothers body to the baby.
LLLI says, “Those who become infected shortly before giving birth and then begin breastfeeding, and those who become infected while breastfeeding, will produce specific secretory IgA antibodies and many other critical immune factors in their milk to protect their nursing infants and enhance their infants’ own immune responses. At this time, these immunologic factors will aid their infants’ bodies to respond more effectively to exposure and infection. Following good hygiene practices will also help reduce transfer of the virus.”
For more information on pregnancy and birth in relation to COVID-19 (coronavirus), please visit the CDC here.

Feb 24, 2020 | Birth
The nursery is ready, you’ve gotten everything on your baby registry, and your pregnancy is nearing full term. But do you know how to labor effectively and push baby out?
We tend to over prepare for our babies’ arrival in ways that help us when we’re past the finish line, in postpartum. That’s all well and good, but we need to get ready for those last few miles of pregnancy, too. I’m likening pregnancy and labor to a marathon because it is! Actually, it’s even harder. Don’t worry, though. You’re tougher than all of it.
If runners have to train, be knowledgeable about their bodies and have the right tools to finish their marathon, then so do you! It’s important to be educated about labor and birth so you can be more prepared. Just picture it – you’ve been in labor for quite a while. Then your care provider tells you it’s time to push. You’re mentally, emotionally and physically tired. You can see the finish line but it’s one mile uphill. You may be tempted to tell your care provider to go do something unsavory. But you won’t – because you will know exactly what you’ll need to do next.
BEAR DOWN
Have you heard this phrase? You probably have A LOT lately. You’ll be ready to push when you reach 10 cm dilation and feel a lot of pressure on your vagina and rectum, almost like you really need to poop (I know, gross, but it’s true). It’s at this point that you’ll want to bear down (exert pressure) and push.
BREATHING
via GIPHY
We’ve all seen “hee, hoo, hee, hoo” breathing in TV and movies during birth scenes. This type of restricted breathing was popularized by Lamaze. However, Lamaze stopped teaching it in the 1980s, so popular culture needs to quit it with this one.
Evidence shows us that the most effective way to breathe during labor and pushing is whatever is most comfortable for the mom. Diaphragmatic, or belly, breathing is usually a very pleasant breathing technique for women during labor. When you feel a contraction coming on during pushing, try to take in a breath and then try to slowly release it while you bear down. Do whatever works best for you!
BE PREPARED
Don’t run your marathon without getting ready. There’s so much more to learn about labor and birth. Get all the tools and knowledge you’ll need by taking a childbirth education course. You’re almost there! You’ll be in labor soon enough.

Jan 13, 2020 | Postpartum
You’ve done it! Congrats on your baby, mama! Be proud of what you’ve accomplished. Now it’s time for postpartum care.
Your care provider or childbirth educator may warn you about how you could feel after delivery. If you had a vaginal delivery, you’ll experience swelling around your vagina and perineum. Tearing is pretty common during birth, but there are varying degrees of severity. Third and fourth degree tears (the most severe) are less common, thankfully! And, I’m sorry to say, many of us will experience hemorrhoids from pushing. Every mama needs to take it easy to heal up.
I know this sounds scary. These discomforts, especially after being pregnant and uncomfortable, can be difficult. But you can get prepared for postpartum and what you’ll need to get through those first few weeks of healing.
Here are my top four postpartum care products for vaginal delivery.
1. Ice Diapers
 Hear me out – many maternity wards make these for new moms. Take a Pampers diaper and pull apart the top of the diaper. Fill it with ice chips. Then fold the open top and use the sticky tabs of the diaper to close. Watch directions here. This goes right in your underwear and IT WILL FEEL AMAZING.
Hear me out – many maternity wards make these for new moms. Take a Pampers diaper and pull apart the top of the diaper. Fill it with ice chips. Then fold the open top and use the sticky tabs of the diaper to close. Watch directions here. This goes right in your underwear and IT WILL FEEL AMAZING.
I had a second degree tear that was very close to being a third degree. Ice diapers were the only things that could completely numb my perineum and vagina. These were the most helpful in my postpartum care. The ice greatly helps reduce swelling after delivery. Another option if you don’t like the ice diaper is to make a padsicle – soak a maxi pad in witch hazel and stick it in the freezer for some nice cold pain relief.
 You may find a can of Dermoplast in your hospital room after delivery. It’s used to spray your perineum to cool and help numb any pain from swelling and hemorrhoids. The spray’s cooling effect provides some temporary relief. This was one of my go-tos after vaginal delivery.
You may find a can of Dermoplast in your hospital room after delivery. It’s used to spray your perineum to cool and help numb any pain from swelling and hemorrhoids. The spray’s cooling effect provides some temporary relief. This was one of my go-tos after vaginal delivery.
Another important product in my postpartum care kit for new moms is Tucks Pads. They are medicated with witch hazel to help relieve, you guessed it, hemorrhoids. But I found its cool temperature great for the perineum, as well. You can put them on your pad or panty liners.
4. Disposable Underwear
While I never saw myself wearing Depends until I reached ripe old age, using disposable underwear was the best advice I got from another mom. Women often bleed for several weeks after birth and may have trouble controlling pelvic muscles and actions, including peeing. A cough or sneeze, and like in pregnancy, a wee bit of wee may come out. I was so glad that I didn’t have to worry about my good underwear during postpartum. If I moved around too much one day and my bleeding got worse or I all of a sudden felt the urgent need to pee and wasn’t sure I’d make it to the bathroom, my disposable underwear had me covered.
Postpartum’s not glamorous for sure, but these items will definitely help get you recover from birth. If you want to learn more about what to expect from birth and postpartum, check out my Informed and Mindful Birthing online class.



 The
The 
 So far, no evidence of the virus has been found in breast milk.
So far, no evidence of the virus has been found in breast milk. 

 Hear me out – many maternity wards make these for new moms. Take a Pampers diaper and pull apart the top of the diaper. Fill it with ice chips. Then fold the open top and use the sticky tabs of the diaper to close.
Hear me out – many maternity wards make these for new moms. Take a Pampers diaper and pull apart the top of the diaper. Fill it with ice chips. Then fold the open top and use the sticky tabs of the diaper to close.  You may find a can of Dermoplast in your hospital room after delivery. It’s used to spray your perineum to cool and help numb any pain from swelling and hemorrhoids. The spray’s cooling effect provides some temporary relief. This was one of my go-tos after vaginal delivery.
You may find a can of Dermoplast in your hospital room after delivery. It’s used to spray your perineum to cool and help numb any pain from swelling and hemorrhoids. The spray’s cooling effect provides some temporary relief. This was one of my go-tos after vaginal delivery.
Recent Comments