
Oct 27, 2020 | Infant Care, Postpartum

Bella, Nurturing Lift, LLC
A Bit About Bella and OT
Hi Mamas! So excited to be writing to you this week. Before we jump into infant development and milestones, I figured I’d give you a little blurb about me. I’m Bella – an occupational therapist and Tummy Time expert on Long Island that specializes in women’s health and infant/pediatric development. Now, many of you may be wondering, what is an occupational therapist (OT)? We’re kind of like the Swiss Army Knives of health care professionals – plug us into whatever scenario/setting/client population, and our skill sets may vary a bit. BUT at the heart of every OT is this notion…our goal is to facilitate you – our client – living your life to your fullest by doing what is most meaningful to YOU! For my private practice, mama and little one are both my clients. Although I specifically make a plan of care with you around lactation and/or infant feeding, I also recognize that we are the sum of our parts, and that you both are your own individuals.
Infant Milestones
So, with introductions out of the way, let’s jump into the topic of “Infant Milestones.” This post isn’t your traditional guide on development (although there will certainly be tips and tricks throughout). What I am hoping you take away from this is confidence and perspective. As parents, we all want our children to thrive – but it’s so important to respect that thriving looks different for every little one. Of course, we want to meet their basic needs (food, clean diapers, shelter, love). We also want to remember that they are their own little person, with likes and dislikes, feelings, personalities – just like you and me!
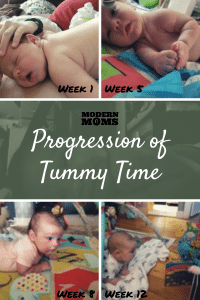
Tummy Time – Am I Doing This Right?
Let’s take a look at “Tummy Time” for example. As a pediatric OT, I constantly see parents bombarded by so many messages from other parents, pediatricians, and Dr. Google on “How to do Tummy Time the right way”. How overwhelming is that?! Especially if your little one hates Tummy Time (gasps). There is no cookie-cutter “right” way, mama! There are two very helpful concepts that can be invaluable for approaching Tummy Time: flexibility and opportunity.
Flexibility
Just like you or I may change what we are in the mood for or to do, so can babies! One day – even one hour – little one may be all about playing on his or her tummy; the next time, not so much. It’s the general trend that we’re looking to be consistent. Which brings me to the next concept —
Opportunity

Courtesy of Nurturing Lift, LLC
Although well-meaning, many pediatricians and health care professionals may stick to this idea that little one HAS to do Tummy Time for “x” amount of minutes a day. That notion is too inflexible, and oftentimes leaves parents feeling overwhelmed when they can’t meet that rigid criteria. So, there’s a growing movement of us that recommends ditching the clock and don’t worry about minutes. You heard me – stop looking at the clock, mama! Instead, it’s about providing our little ones with the opportunity for Tummy Time and floor play. What Tummy Time looks like depends on your baby’s age (check out the pictures) and preferences. A starting place may be four opportunities on a daily basis for baby to have for floor play. Each of those sessions may look different – which is where the flexibility comes into play.
Encouraging Positive Experiences
I truly believe that we as parents become the experts when it comes to our children. Recognizing our little ones’ stress cues can make infant development and promoting milestones much more of a tolerable (and even pleasant) experience. We want to try to catch these cues before we get to later cues like crying. They may look like baby starting to avoid your eye contact; skin color changes (reddened eyebrow areas); yawning; frantic squirming; and more. When you start to notice these cues, it can indicate baby is nearing the end of this activity (and is moving toward a state where there is too much stimulation in their environment).
This is where we help guide our little ones towards resilience. Instead of picking them up right away and removing them immediately from the situation, try helping them exit the situation themselves. The primary example I give is when baby is done with Tummy Time gently helping guide their shoulders and hips, showing them that they can start to get back onto their backs. Resilience in the face of adversity is one of the most invaluable skills we can help our children with.
Manageable Milestones
I can go on and on about infant development, but I would not want the above message lost! I hope that this post left you feeling like baby milestones looked less like mountains and appeared much more manageable. If you have any questions, please feel free to reach out. You got this, mama! And thank you, Cassie, for giving me a place to help get this message out!
Love & Positivity,
Bella
ABOUT: Gabriela Masotti Rochford, MSOT, OTR/L, Certified Breastfeeding Specialist ™️. Contact Bella at Nurturing Lift, LLC
**Disclaimer: Remember that EVERY baby is different. Little one in these pictures is meant to show you the somewhat linear way that we would like the trajectory of infant motor development to go with Tummy Time. If you are concerned about your child’s milestones (e.g. 6 month old unable to lift head up from floor or roll in at least one direction), reach out to your pediatrician as well as a pediatric development specialist (OT or PT) to assess for whether your little one may benefit from early intervention services**

Sep 3, 2020 | Postpartum, Uncategorized
Finding My Postpartum Village
I didn’t understand how true the saying “It takes a village” really is and how badly I needed that village in postpartum. While as a birth educator I know preparing for labor and birth is very important, I didn’t spend nearly as much time preparing for what comes after. Sure, I got the breast pump, nursing pads, mesh underwear, perineal spray, etc. All of those items were helpful. But what I needed, what I really needed, I couldn’t buy on Amazon.
Support. A community of other new moms going through the same challenges, joys, feelings I was going through. This is what I was missing. Although I had my close friends and family, I still felt a bit isolated because no one else was experiencing postpartum with me. In a way I was alone and at the time I didn’t realize that I didn’t have to feel like that. I was stubborn to opening up and asking for more help.
Postpartum Requires Support
 At around four months postpartum, I received an invitation to the Fourth Trimester Support Group at The Nesting Place from part owner and colleague Laura Siddons. She asked if I’d like to sample the group to see what it’s all about not just for future postpartum clients, but also for myself as a new mom. The group was around 45 from me and I was suffering a lot of anxiety while driving. I let my anxiety get in the way of going for a while, but eventually I did make it to a group meeting and what I found was an amazing group of friendly, supportive moms, a generous host, and a knowledgeable guest expert. In that meeting alone, I learned baby massage techniques that helped greatly soothe my baby before bed and made life much easier for me.
At around four months postpartum, I received an invitation to the Fourth Trimester Support Group at The Nesting Place from part owner and colleague Laura Siddons. She asked if I’d like to sample the group to see what it’s all about not just for future postpartum clients, but also for myself as a new mom. The group was around 45 from me and I was suffering a lot of anxiety while driving. I let my anxiety get in the way of going for a while, but eventually I did make it to a group meeting and what I found was an amazing group of friendly, supportive moms, a generous host, and a knowledgeable guest expert. In that meeting alone, I learned baby massage techniques that helped greatly soothe my baby before bed and made life much easier for me.
Since I visited the group, I’ve been able to cultivate my own supportive village out of friends, colleagues, and new moms. I know who I can message at any time during the day when I have a question about my growing baby (now toddler), parenting tips, or when I just need to vent.
I’m so glad I found support. I am a stubborn person who has trouble asking for help, but my experience helped bring down those walls, allow me to get what I need, and learn how to give others that postpartum support freely with compassion and love.
Find Your Support
I’m so excited to now be facilitating a Fourth Trimester Support Group starting September 16. Reserve your spot and start your journey of finding your motherhood village.
With love,
Cass

Jul 14, 2020 | Postpartum
Let’s Talk About It
The pelvic floor often gets ignored during regular checkups in postpartum, but are vital to our sexual and reproductive health. I talked about pelvic floor muscles during pregnancy in my previous blog post and now it’s time to talk about some of the nitty gritty details of pelvic health and postpartum. While our bodies expand and change in beautiful and often uncomfortable ways during pregnancy, they also go through A LOT during labor and birth. Our perineum has to stretch during vaginal birth and that, along with tearing, can have an impact on your pelvic floor health in postpartum and beyond.
Many new moms experience pelvic floor issues after vaginal birth and don’t seek treatment because women’s health is often stigmatized. So let’s talk about it! It’s the only way to push back and normalize the experiences of birthing people.
Once again, I reached out to Dr. Rachel Parrotta, DPT, for her take.
What’s Normal

Certain exercises like this bridge can help strengthen core and pelvic muscles
“The pelvic floor muscles undergo a very large stretch during vaginal birth and the pelvic region can be quite swollen in the first few weeks post-partum,” said Dr. Parrotta. “These factors can make it very challenging to coordinate your pelvic floor muscles (aka ‘Find your Kegel’) in the first few weeks after birth. Learning and practicing pelvic floor muscle coordination prior to birth can help develop ‘muscle memory’ that will assist you in postpartum recovery.”
I have oft heard phrases like “birth will wreck your vagina” said to new moms and it’s untrue. As Dr. Parrotta mentioned, the vagina and pelvic muscles largely expand. But, here’s the thing – they are meant to do this. After vaginal birth, your pelvic floor is bound to be swollen and aggravated. So, it’s completely normal to experience some postpartum incontinence and perineal discomfort in the following weeks.
What’s Not Normal
If you experience any of the following after you’re six-weeks pospartum, visit your care provider and seek out a pelvic health specialist:
- Pain during sex
- Perineal pain
- A heavy feeling or pressure in your perineal area
- Incontinence
- Difficulty urinating or passing a soft bowel movement
Final Thought
Your pelvic health is important. A healthy pelvic floor after postpartum can lead to better sexual satisfaction for you, more stability in your pelvic region, and better outcomes in future pregnancies.
Pelvic PT can be intimate, but it shouldn’t feel invasive. Find a practitioner you trust and get evaluated, because your health is worth it.

May 18, 2020 | Postpartum
I’m a postpartum doula on Long Island. The first response I get when I tell someone this is, “What is a postpartum doula? What do you do?” The answer is quite simple  and the service is a life-saver for many.
and the service is a life-saver for many.
Mothering The Mother
My job is to help Long Island postpartum moms who have recently birthed or adopted a baby. I help them cope, adjust, heal, and feel confident in their parenting. How do I do this? Well, I provide a myriad of services that combine into a practice of care and support.
The first tenant of being a postpartum doula is to “Mother the Mother.” Us doulas believe that every mama deserves to be nurtured with compassion; so, our role is to give motherly love and support. We don’t replace any client’s mom or other family member. In fact, we often work hand-in-hand with our clients’ family members to give as much help as possible.
What Services Postpartum Doulas Provide
 The types of services a postpartum doula does will depend on the doula. I provide full spectrum care to moms, which includes the following:
The types of services a postpartum doula does will depend on the doula. I provide full spectrum care to moms, which includes the following:
1. Emotional and physical support for mom
2. Postpartum care – help with healing and perineum care, c-section support, rest, and sleep
3. Infant care – educate the whole family on baby care best practices, help with bathing, sleep, feeding, and more
4. Feeding education – breast and formula
5. Nutrition – guidance for healing and lactation, meal and snack preparation
6. Household chores – light tasks such as washing dishes, doing laundry for the whole family, kitchen cleanup, and organizing the baby’s room
7. Family support – help partners and older children adjust to new family dynamic
8. Mental health – I’m trained to educate and identify perinatal mood and anxiety disorders such as postpartum depression and anxiety
9. Overnight care – I’ll take care of your baby’s needs throughout the night including diaper changes, bringing baby to you for breastfeeding, bottle feeding, and comforting baby so you can get a good night’s sleep
I do all this and even more!
What Postpartum Doulas Don’t Do
Postpartum doulas are not medical health providers. While we can provide evidence-based information on care, we aren’t doctors and cannot answer medical questions. When appropriate, we will refer clients to their pediatricians.
Sometimes people assume we are just like babysitters. However, our job is to put the mom first, not baby. Postpartum doulas will often watch over the baby so that mom can get some rest. But, we don’t completely take over care for extended periods of time unless we are providing overnight care. More importantly we are highly trained professionals that receive certification credentials.
We also typically do not do heavy cleaning like vacuuming, washing the floors, cleaning the bathroom, etc.
Learn More
Are you a Long Island mom looking for support? Contact me or learn more about postpartum care here.

Mar 17, 2020 | Mental Health, Postpartum, Pregnancy
Isolation can be a real trigger for depression, especially since so many of us are now practicing social distancing and self quarantine because of COVID-19 (coronavirus). Pregnant and new moms, in particular, can be at-risk of prenatal and postpartum mood and anxiety disorders (PMADs). Just because we’re stuck home, doesn’t mean we have to do it all alone!
While things will return to normal eventually, here are five things you can do today to help prevent isolation depression and anxiety.
1. Virtual Support
Many birth workers and care providers are adapting to the current situation by providing virtual support via web chat. There are apps that provide chat and over-the-phone access to therapists. You can look for a pregnancy or postpartum support group online, like this one from The Nesting Place.
Birth and postpartum doulas are also offering online care. I’m still able to chat with clients, show them newborn care basics, help with lactation, and provide emotional support and encouragement. If you’re interested in getting a postpartum doula virtually, contact me.
You can also talk to friends and family members via Skype, Facetime, Facebook chat, or on the phone to avoid feeling alone.
2. Get Some Fresh Air
If you’re able, sit outside in your backyard or balcony for a while. Get some fresh air and Vitamin D. Just getting outside, without running into other people, can be so refreshing and uplifting. If you live in an apartment and can’t leave, but the weather isn’t too chilly, try opening the windows for a little while. Let in the sunshine. Take in its warmth for a moment. Nature can offer some relief.
 3. Exercise
3. Exercise
Get those endorphins pumping! If you’re pregnant or in postpartum and cleared for gentle exercise, stream some prenatal workouts on YouTube. Prenatal yoga and meditation can be calming. You don’t have to exercise all day, but even twenty minutes can make a big difference in how we feel. If you’re new to yoga, check out this YouTube workout for beginners.
4. Read
Reading is a total immersive experience that’s good for your brain! Stories can transport you out of your current environment. According to a study by Emory University, reading activates neurons in the brain that create a sensation of not just reading about the action of the book, but experiencing the sensations it is describing. You are figuratively and biologically put in the shoes of another. This is called grounded cognition.
Reading can also help to calm the mind and help it focus if you’re feeling anxious.
5. Find and List Resources
Sometimes just being prepared helps us feel more calm and in control. Do some research on local and other online resources you may want to use during this time like restaurants that are still doing delivery, your care providers’ emergency numbers and assistance programs in your area. You don’t have to use any of these if you don’t need to, but having a list of people to call may help you feel more connected. Many of us are isolated at this moment. It’s important to remember that there are networks of people in every community that are still out there to help you.
Sending you love through this difficult time!
Cass

Mar 13, 2020 | Birth, Postpartum
Tensions about COVID-19, a type of coronavirus, are rising in the United States as the illness has been spreading. Travel is becoming restricted, people are working from home, schools are closing, and apparently toilet paper is now a hot commodity. Many are starting to panic. The symptoms of COVID-19 have mainly proven to be more serious in older patients and those with serious complications such as heart and lung disease, and diabetes. But what about pregnant women and new moms?
Are Pregnant Women More Susceptible to Getting COVID-19 or at Higher Risk of Serious Illness?
At this time, the CDC does not have conclusive information. However, the physiological changes women experience during pregnancy do tend to make them more susceptible to viral respiratory infections. The CDC advises pregnant women to take standard precautions like washing their hands and avoiding other people who are sick.
Can COVID-19 be Transmitted to Babies During Pregnancy or Vaginal Birth?
The virus is currently thought to only be spread through respiratory droplets, meaning through fluids expelled by the mouth and nose during coughs, sneezes or intimate contact. It is unknown if the virus can be transmitted through the womb. However, the CDC said, “In limited recent case series of infants born to mothers with COVID-19 published in the peer-reviewed literature, none of the infants have tested positive for the virus that causes COVID-19. Additionally, virus was not detected in samples of amniotic fluid or breastmilk.”
Can I Continue Breastfeeding?
 So far, no evidence of the virus has been found in breast milk. La Leche League International (LLLI) advises women to continue breastfeeding unless a care provider deems it medically necessary to stop. Human milk provides important immunological antibodies produced in the mothers body to the baby.
So far, no evidence of the virus has been found in breast milk. La Leche League International (LLLI) advises women to continue breastfeeding unless a care provider deems it medically necessary to stop. Human milk provides important immunological antibodies produced in the mothers body to the baby.
LLLI says, “Those who become infected shortly before giving birth and then begin breastfeeding, and those who become infected while breastfeeding, will produce specific secretory IgA antibodies and many other critical immune factors in their milk to protect their nursing infants and enhance their infants’ own immune responses. At this time, these immunologic factors will aid their infants’ bodies to respond more effectively to exposure and infection. Following good hygiene practices will also help reduce transfer of the virus.”
For more information on pregnancy and birth in relation to COVID-19 (coronavirus), please visit the CDC here.




 At around four months postpartum, I received an invitation to the
At around four months postpartum, I received an invitation to the 


 and the service is a life-saver for many.
and the service is a life-saver for many. The types of services a postpartum doula does will depend on the doula. I provide full spectrum care to moms, which includes the following:
The types of services a postpartum doula does will depend on the doula. I provide full spectrum care to moms, which includes the following:
 3. Exercise
3. Exercise
 So far, no evidence of the virus has been found in breast milk.
So far, no evidence of the virus has been found in breast milk.
Recent Comments