
Nov 10, 2021 | Pregnancy
You’re pregnant, working full-time, taking care of family and friends, dealing with a pandemic, and struggling to balance it all while feeling exhausted and trying to survive morning sickness. Sound familiar? If you’re nodding your head going, “Yes, OMG I’m dealing with all of this” you’re not alone, but you’re probably feeling pretty stressed. Could it be possible that all these high levels of stress are causing your difficult pregnancy symptoms?
 What are normal symptoms in pregnancy?
What are normal symptoms in pregnancy?
There are normal discomforts that come with pregnancy – morning sickness, fatigue, headaches, back pain, heartburn, and more. You’ve probably heard your friends, family, and doctors saying that what you’re feeling is just par for the course. However, this is not always the case. Sometimes there’s a different underlying cause that’s not being addressed, especially when difficult symptoms continue beyond an expected time or become debilitating.
What is the impact of stress?
Experiencing high levels of stress over a longer period of time is called chronic stress. This condition can actually cause a lot of the same symptoms associated with pregnancy, such as:
- Fatigue
- Nausea and digestive issues
- Headaches
- Difficulty concentrating
- Aches and pains
- Feeling irritable
- Mood swings
- Constantly thinking or worrying. Can’t shut your brain off
- High blood pressure
In addition to all this, chronic stress in pregnancy can cause preterm labor and impact your baby’s health.
These symptoms can often be mistaken for normal pregnancy ailments. But they can also, in turn, cause more stress and create a cycle of anxiety tied to physical health issues. What you feel is valid and there is a reason behind it.
If you’re experiencing difficult pregnancy symptoms due to chronic stress, there are ways to relieve these symptoms, feel healthier, and enjoy your pregnancy.

Nov 4, 2021 | Pregnancy
You’ve seen the words repeated in articles and said multiple times in your OB or Midwife’s office – folic acid, folate, folic acid, folate. These words are often used interchangeably, but they are not the same. So, what is the difference between the two and what’s the craziest hidden benefit of folate vs folic acid for mom and baby?
______________________________________________________________________________
 Relieve Your Miserable Pregnancy Symptoms in 5 Days
Relieve Your Miserable Pregnancy Symptoms in 5 Days
Free virtual retreat Nov 13-17
Live your best baby bump life and get rid of those pregnancy symptoms that are making you feel miserable. Fatigue, morning sickness, pelvic pain, and more!
________________________________________________________________________________
What is folic acid and folate?
Folate and folic acid are names for vitamin B9, an essential vitamin our bodies need for healthy cell and DNA growth. When we consume vitamin B9, our bodies need to convert it into the active form of B9 called levomefolic acid as it enters our bloodstream. While both names refer to the same vitamin, there is a key difference.
 Folate is a naturally occurring form of B9, while folic acid is a synthetic form.
Folate is a naturally occurring form of B9, while folic acid is a synthetic form.
So, which is better?
Because folate is natural, our bodies convert most of it into that active form in our bloodstream. We need to get the true benefit of the vitamin. However, the body cannot break down and convert most of the folic acid in the bloodstream. So, it stays there for longer until it can get processed in the liver. This results in a possible build up of folic acid in the body, which can cause health issues like increasing the risk of cancer.
I wonder why they even sell it, especially to pregnant women.
The benefit of folate far exceeds that of folic acid.
Why do I need folate during pregnancy?
Pregnant people need folate especially to prevent birth abnormalities like neural tube defects, which have been linked to low levels of vitamin B9.
You can get folate through a supplement and by eating dark, leafy greens like spinach and brussel sprouts.

Nov 3, 2021 | Uncategorized
Your baby bump is growing. How exciting! You’re finally showing off that adorable bump, but you’re starting to notice that a bigger bump comes with more aches and pains, especially in your back. Don’t despair – I’m going to share the one surprising thing that completely helped me and can improve your pregnancy back pain.
Why Does Your Back Hurt So Much?
Our growing babies are stretching the muscles around our bellies, pulling our round ligaments in our groins and around our backs. The more our bumps grow, the more weight and pulling of our muscles. Plus, your baby may be laying more on your spine. Perhaps your baby is in the posterior position, aka sunny side up, and putting even more of its weight on your back. All of this is going to cause achiness and pain.
But, this doesn’t mean you need to suffer needlessly. So, how can you improve your pregnancy back pain?
______________________________________________________________________________
 Relieve Your Miserable Pregnancy Symptoms in 5 Days
Relieve Your Miserable Pregnancy Symptoms in 5 Days
Free virtual retreat Nov 13-17
Live your best baby bump life and get rid of those pregnancy symptoms that are making you feel miserable. Fatigue, morning sickness, pelvic pain, and more!
________________________________________________________________________________
The One Trick That Helped Me
This one thing will not cost you any money. I had bought a pregnancy belly band to help with my round ligament pain, and it did provide some relief while I was at work, but it didn’t help with my back pain.
 My chiropractor, Lisa Lipari, suggested I try pelvic tilts to ease my back pain. What are pelvic tilts? If you do yoga, you may know them as the Cat/Cow pose. And it made a huge difference in my pregnancy.
My chiropractor, Lisa Lipari, suggested I try pelvic tilts to ease my back pain. What are pelvic tilts? If you do yoga, you may know them as the Cat/Cow pose. And it made a huge difference in my pregnancy.
This movement requires you to be on all fours and tilt your pelvis downward toward the floor and back up, almost forming a straight table with your spine. Don’t tilt your pelvis all the way up to the ceiling like you would in yoga.
I did this move several times a day, but especially right before bed. I couldn’t sleep because my back was so uncomfortable, but once I started doing 20 sets of these beforehand, my pain was at ease and I could sleep! Try doing the same before bed every night.
BONUS – this move is wonderful for improving your pelvic floor and having a smoother labor!
*As always, ask your doctor if you’re cleared for exercise before attempting this stretch*

Oct 8, 2021 | Coping Skills, Mental Health, Pregnancy
Pregnancy can be stressful. While some pregnant people feel calm throughout all three trimesters, others are not as lucky. If you’re like me, struggling to relax and feeling the physical symptoms of stress, you may be wondering what steps to reduce stress while pregnant you can take.
Stress can make us feel horrible in general. It can cause headaches, nausea, difficulty concentrating, and more. During pregnancy, stress can lead to the same symptoms that may be written off as common pregnancy ailments. But you don’t have to accept this suffering. There are plenty of steps you can take to reduce your stress and the symptoms that come with it.
Step 1: Find Your Triggers
There are many factors that can lead to moderate and high levels of stress like work, family, finances, environment, grief, food, and big life changes such as pregnancy.
Identifying where your stress is coming from is key to undoing it and reducing stress while pregnant. Sit down, make a list of everything that’s on your mind. Reflect on your environment, relationships, and career. What is making you feel anxious?
Step 2: Practice Stress Reduction Techniques
Stress will not go away on its own. Instead, it will fester and increase the severity of symptoms over time.
 So, it’s important to practice stress reduction techniques like mindfulness and self-care. That’s why I created my 5 Day Pregnancy De-Stress Challenge. Every day starting October 18, participants will receive a self-care activity that will let them indulge in relaxation and ease pregnancy discomforts from stress (It’s not too late to sign up! Click here to join or sign up below).
So, it’s important to practice stress reduction techniques like mindfulness and self-care. That’s why I created my 5 Day Pregnancy De-Stress Challenge. Every day starting October 18, participants will receive a self-care activity that will let them indulge in relaxation and ease pregnancy discomforts from stress (It’s not too late to sign up! Click here to join or sign up below).
Step 3: Make a Plan
Incorporating stress reduction techniques and self-care will help minimize and cope with symptoms of stress. However, the root of the issue (your stress trigger) may still exist. Perhaps your trigger is a situation that isn’t easily fixed or is long-term. That’s okay. It’s natural to be overwhelmed. But, you can still make a plan either with your partner, family, health coach, care provider, etc to take actionable steps for coping or working toward solving what’s causing your stress.
So, here it is – three steps to reduce stress while pregnant. De-stressing isn’t always easy and doesn’t happen overnight. But learning to put your well-being first, can make a difference.
If your stress leads to feelings of depression or severe anxiety, it’s never too late to consult a maternal mental health professional for help.

Sep 22, 2021 | Uncategorized
You’re pregnant! Hooray! And even better, you’ve gotten through the first trimester’s dreaded morning sickness period. Hopefully by now, your stomach is taking it easier on you and you’re starting to eat more normally, or even getting some cravings. Either way, I know you’ve heard the phrase “Eating for two.” It’s often misinterpreted as the ability to each twice as much during pregnancy. Don’t get me wrong – you DO need more calories every day through pregnancy. Roughly 300-500 calories per day depending on your pregnancy weight management. What I don’t like about this term is when it is stereotypically used, or as a joke because of pregnancy weight gain.
There can be a lot of feelings of guilt and shame for moms-to-be, especially plus size mamas. Whatever your body shape, I don’t want you to ever feel bad for eating. You need to eat for your well-being. So, let’s change the meaning behind “eating for two.”
What Eating for Two Means to Me
The phrase traditionally refers to the portion size aka amount of food. To me, eating for two means nourishing yourself and your baby. But, not in the manner of eating double the portions. Instead, you’re eating the nutrients and delicious meals you need to effectively create the building blocks of your baby’s life and support your own well-being. What you eat is also what your baby’s eating. I want you both to have the best of what you need. Quality over quantity.
Are you stress eating? Take my pregnancy stress quiz to uncover your stress levels and get a personalized plan for addressing stress.
Look, you don’t have to constantly eat a salad. That’s not what I’m saying here. It’s totally okay to enjoy that slice of pizza or some ice cream. You don’t need to deny yourself pleasures as long as they fit within the parameters of your pregnancy and your care provider hasn’t restricted your diet. But, the goal before occasionally indulging is to get the other foods you need for a healthier and more comfortable pregnancy.
 What Do You Need to Eat for a Healthy Pregnancy?
What Do You Need to Eat for a Healthy Pregnancy?
Let’s break it down. First and foremost, you need protein, and there are lots of ways to get it even if you’re a vegetarian or are vegan. You need healthy, complex carbs from whole grains and multigrains. Simple carbs like white bread and those in a lot of products in the snack aisle are going to break down into extra sugar, while complex carbs will provide some protein, fiber, iron, and more! You need healthy fats, omega-3s and omega-6s, as well as more fiber (for that pregnancy constipation).
When you can get all these essential nutrients into your diet, you and your baby will feel nourished and supported.
Learn more about having a healthy pregnancy here.

Aug 27, 2021 | Pregnancy
Common Plus Size Pregnancy Discomforts
Pregnancy, while a wonderfully joyous time, can also be full of stress and physical discomforts. Our bodies are drastically changing by the moment to accommodate the little life growing inside. If you were expecting that gorgeous pregnancy glow, only to be spending a lot more face time with your toilet, you are not alone. I thought I would feel like a goddess, but instead I had extreme nausea, fatigue, and aches and pains. Also, as a plus size mom my discomfort was even higher because of the extra weight I gained during pregnancy. What I didn’t know then was that there are solutions that could have helped ease these discomforts. So, here are 3 common plus size pregnancy discomforts and the remedies to help you.
 Nausea
Nausea
Ah, yes. The oft-spoke about morning sickness. Some are lucky to not experience much nausea or vomiting in the first trimester. If you’re not one of those people (I feel you), here are some things you can do:
- Eat small, frequent meals. (Tip: we often crave carbs when we’re nauseous. Opt for whole wheat or whole grain options to avoid simple, sugary carbs. Plus, whole grains have more fiber! See below for why that’s an added bonus)
- Take vitamin B6. Several studies have shown that this essential B vitamin significantly decreases nausea and vomiting in pregnant women. In fact, vitamin B6 makes up 50% of the ingredients of a popular prescription for nausea and vomiting for pregnant women, Diclegis. **Ask your doctor before taking any supplements**
- Wear motion-sickness wristbands.
- Sip clear fluids. Sugar-free flavored or plain seltzer is a great go-to. I LOVED using my S’well bottle during pregnancy. It kept my drink cold all day long. Luckily, S’well is having a Labor Day Sale: 25% off sitewide! Valid 9/2-9/6.
 Take advantage while you can!
Take advantage while you can!
Body Aches
Baby is growing, which means you are too! Our muscles are being stretched and pulled in all different directions and the baby is getting heavier every week, so it’s only natural to be feeling achy. You don’t have to grin and bear it. You deserve to be as comfortable as possible. Here are my suggestions:
- Prenatal yoga. If you can, prenatal yoga classes help keep our muscles strong, our bodies balanced, our stress lower, and our muscles stretched. **Ask your doctor which types of exercise are right for you and your pregnancy**
- Prenatal massage. Get pampered, mama! After the first trimester, it is generally considered safe to get a prenatal massage from a qualified masseuse. Or ask your partner or friend to give you a light massage.
- Belly support. As your belly grows, we can start to feel more back and ligament pain. Buying a belly band or having your doula or midwife assist you with belly wrapping (either with cloth or tape) can help your body better support your baby’s weight, and ultimately, help ease those pains.
- Drink more water. Hydration helps those crampy muscles.
- Warmth. A warm bath or compress on the area that’s bothering you could help give you relief
- Maternity pillow. This is worth the investment. The further along we get, especially in the third trimester, the more uncomfortable we may feel and the harder it is to sleep at night. Having a maternity pillow to cradle your belly and cushion between your legs, taking the pressure off your spine, can make your nights, and days, more comfortable.
 Constipation
Constipation
Our babies need a lot of room, which means our intestines have much less room. Constipation can cause A LOT of discomfort in your lower belly. The bloating, the cramping – the struggle is real. Here are my tips to get things moving:
There are many solutions and alternatives to try to ease common plus size pregnancy discomforts. Sometimes it’s a matter of trial and error, but the most important thing is helping you be as comfortable as possible.

Oct 27, 2020 | Infant Care, Postpartum

Bella, Nurturing Lift, LLC
A Bit About Bella and OT
Hi Mamas! So excited to be writing to you this week. Before we jump into infant development and milestones, I figured I’d give you a little blurb about me. I’m Bella – an occupational therapist and Tummy Time expert on Long Island that specializes in women’s health and infant/pediatric development. Now, many of you may be wondering, what is an occupational therapist (OT)? We’re kind of like the Swiss Army Knives of health care professionals – plug us into whatever scenario/setting/client population, and our skill sets may vary a bit. BUT at the heart of every OT is this notion…our goal is to facilitate you – our client – living your life to your fullest by doing what is most meaningful to YOU! For my private practice, mama and little one are both my clients. Although I specifically make a plan of care with you around lactation and/or infant feeding, I also recognize that we are the sum of our parts, and that you both are your own individuals.
Infant Milestones
So, with introductions out of the way, let’s jump into the topic of “Infant Milestones.” This post isn’t your traditional guide on development (although there will certainly be tips and tricks throughout). What I am hoping you take away from this is confidence and perspective. As parents, we all want our children to thrive – but it’s so important to respect that thriving looks different for every little one. Of course, we want to meet their basic needs (food, clean diapers, shelter, love). We also want to remember that they are their own little person, with likes and dislikes, feelings, personalities – just like you and me!
Tummy Time – Am I Doing This Right?
Let’s take a look at “Tummy Time” for example. As a pediatric OT, I constantly see parents bombarded by so many messages from other parents, pediatricians, and Dr. Google on “How to do Tummy Time the right way”. How overwhelming is that?! Especially if your little one hates Tummy Time (gasps). There is no cookie-cutter “right” way, mama! There are two very helpful concepts that can be invaluable for approaching Tummy Time: flexibility and opportunity.
Flexibility
Just like you or I may change what we are in the mood for or to do, so can babies! One day – even one hour – little one may be all about playing on his or her tummy; the next time, not so much. It’s the general trend that we’re looking to be consistent. Which brings me to the next concept —
Opportunity

Courtesy of Nurturing Lift, LLC
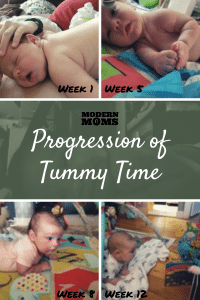
Although well-meaning, many pediatricians and health care professionals may stick to this idea that little one HAS to do Tummy Time for “x” amount of minutes a day. That notion is too inflexible, and oftentimes leaves parents feeling overwhelmed when they can’t meet that rigid criteria. So, there’s a growing movement of us that recommends ditching the clock and don’t worry about minutes. You heard me – stop looking at the clock, mama! Instead, it’s about providing our little ones with the opportunity for Tummy Time and floor play. What Tummy Time looks like depends on your baby’s age (check out the pictures) and preferences. A starting place may be four opportunities on a daily basis for baby to have for floor play. Each of those sessions may look different – which is where the flexibility comes into play.
Encouraging Positive Experiences
I truly believe that we as parents become the experts when it comes to our children. Recognizing our little ones’ stress cues can make infant development and promoting milestones much more of a tolerable (and even pleasant) experience. We want to try to catch these cues before we get to later cues like crying. They may look like baby starting to avoid your eye contact; skin color changes (reddened eyebrow areas); yawning; frantic squirming; and more. When you start to notice these cues, it can indicate baby is nearing the end of this activity (and is moving toward a state where there is too much stimulation in their environment).
This is where we help guide our little ones towards resilience. Instead of picking them up right away and removing them immediately from the situation, try helping them exit the situation themselves. The primary example I give is when baby is done with Tummy Time gently helping guide their shoulders and hips, showing them that they can start to get back onto their backs. Resilience in the face of adversity is one of the most invaluable skills we can help our children with.
Manageable Milestones
I can go on and on about infant development, but I would not want the above message lost! I hope that this post left you feeling like baby milestones looked less like mountains and appeared much more manageable. If you have any questions, please feel free to reach out. You got this, mama! And thank you, Cassie, for giving me a place to help get this message out!
Love & Positivity,
Bella
ABOUT: Gabriela Masotti Rochford, MSOT, OTR/L, Certified Breastfeeding Specialist ™️. Contact Bella at Nurturing Lift, LLC
**Disclaimer: Remember that EVERY baby is different. Little one in these pictures is meant to show you the somewhat linear way that we would like the trajectory of infant motor development to go with Tummy Time. If you are concerned about your child’s milestones (e.g. 6 month old unable to lift head up from floor or roll in at least one direction), reach out to your pediatrician as well as a pediatric development specialist (OT or PT) to assess for whether your little one may benefit from early intervention services**

Sep 3, 2020 | Postpartum, Uncategorized
Finding My Postpartum Village
I didn’t understand how true the saying “It takes a village” really is and how badly I needed that village in postpartum. While as a birth educator I know preparing for labor and birth is very important, I didn’t spend nearly as much time preparing for what comes after. Sure, I got the breast pump, nursing pads, mesh underwear, perineal spray, etc. All of those items were helpful. But what I needed, what I really needed, I couldn’t buy on Amazon.
Support. A community of other new moms going through the same challenges, joys, feelings I was going through. This is what I was missing. Although I had my close friends and family, I still felt a bit isolated because no one else was experiencing postpartum with me. In a way I was alone and at the time I didn’t realize that I didn’t have to feel like that. I was stubborn to opening up and asking for more help.
Postpartum Requires Support
 At around four months postpartum, I received an invitation to the Fourth Trimester Support Group at The Nesting Place from part owner and colleague Laura Siddons. She asked if I’d like to sample the group to see what it’s all about not just for future postpartum clients, but also for myself as a new mom. The group was around 45 from me and I was suffering a lot of anxiety while driving. I let my anxiety get in the way of going for a while, but eventually I did make it to a group meeting and what I found was an amazing group of friendly, supportive moms, a generous host, and a knowledgeable guest expert. In that meeting alone, I learned baby massage techniques that helped greatly soothe my baby before bed and made life much easier for me.
At around four months postpartum, I received an invitation to the Fourth Trimester Support Group at The Nesting Place from part owner and colleague Laura Siddons. She asked if I’d like to sample the group to see what it’s all about not just for future postpartum clients, but also for myself as a new mom. The group was around 45 from me and I was suffering a lot of anxiety while driving. I let my anxiety get in the way of going for a while, but eventually I did make it to a group meeting and what I found was an amazing group of friendly, supportive moms, a generous host, and a knowledgeable guest expert. In that meeting alone, I learned baby massage techniques that helped greatly soothe my baby before bed and made life much easier for me.
Since I visited the group, I’ve been able to cultivate my own supportive village out of friends, colleagues, and new moms. I know who I can message at any time during the day when I have a question about my growing baby (now toddler), parenting tips, or when I just need to vent.
I’m so glad I found support. I am a stubborn person who has trouble asking for help, but my experience helped bring down those walls, allow me to get what I need, and learn how to give others that postpartum support freely with compassion and love.
Find Your Support
I’m so excited to now be facilitating a Fourth Trimester Support Group starting September 16. Reserve your spot and start your journey of finding your motherhood village.
With love,
Cass

Jul 14, 2020 | Postpartum
Let’s Talk About It
The pelvic floor often gets ignored during regular checkups in postpartum, but are vital to our sexual and reproductive health. I talked about pelvic floor muscles during pregnancy in my previous blog post and now it’s time to talk about some of the nitty gritty details of pelvic health and postpartum. While our bodies expand and change in beautiful and often uncomfortable ways during pregnancy, they also go through A LOT during labor and birth. Our perineum has to stretch during vaginal birth and that, along with tearing, can have an impact on your pelvic floor health in postpartum and beyond.
Many new moms experience pelvic floor issues after vaginal birth and don’t seek treatment because women’s health is often stigmatized. So let’s talk about it! It’s the only way to push back and normalize the experiences of birthing people.
Once again, I reached out to Dr. Rachel Parrotta, DPT, for her take.
What’s Normal

Certain exercises like this bridge can help strengthen core and pelvic muscles
“The pelvic floor muscles undergo a very large stretch during vaginal birth and the pelvic region can be quite swollen in the first few weeks post-partum,” said Dr. Parrotta. “These factors can make it very challenging to coordinate your pelvic floor muscles (aka ‘Find your Kegel’) in the first few weeks after birth. Learning and practicing pelvic floor muscle coordination prior to birth can help develop ‘muscle memory’ that will assist you in postpartum recovery.”
I have oft heard phrases like “birth will wreck your vagina” said to new moms and it’s untrue. As Dr. Parrotta mentioned, the vagina and pelvic muscles largely expand. But, here’s the thing – they are meant to do this. After vaginal birth, your pelvic floor is bound to be swollen and aggravated. So, it’s completely normal to experience some postpartum incontinence and perineal discomfort in the following weeks.
What’s Not Normal
If you experience any of the following after you’re six-weeks pospartum, visit your care provider and seek out a pelvic health specialist:
- Pain during sex
- Perineal pain
- A heavy feeling or pressure in your perineal area
- Incontinence
- Difficulty urinating or passing a soft bowel movement
Final Thought
Your pelvic health is important. A healthy pelvic floor after postpartum can lead to better sexual satisfaction for you, more stability in your pelvic region, and better outcomes in future pregnancies.
Pelvic PT can be intimate, but it shouldn’t feel invasive. Find a practitioner you trust and get evaluated, because your health is worth it.

Jul 2, 2020 | Birth
Pelvic What?
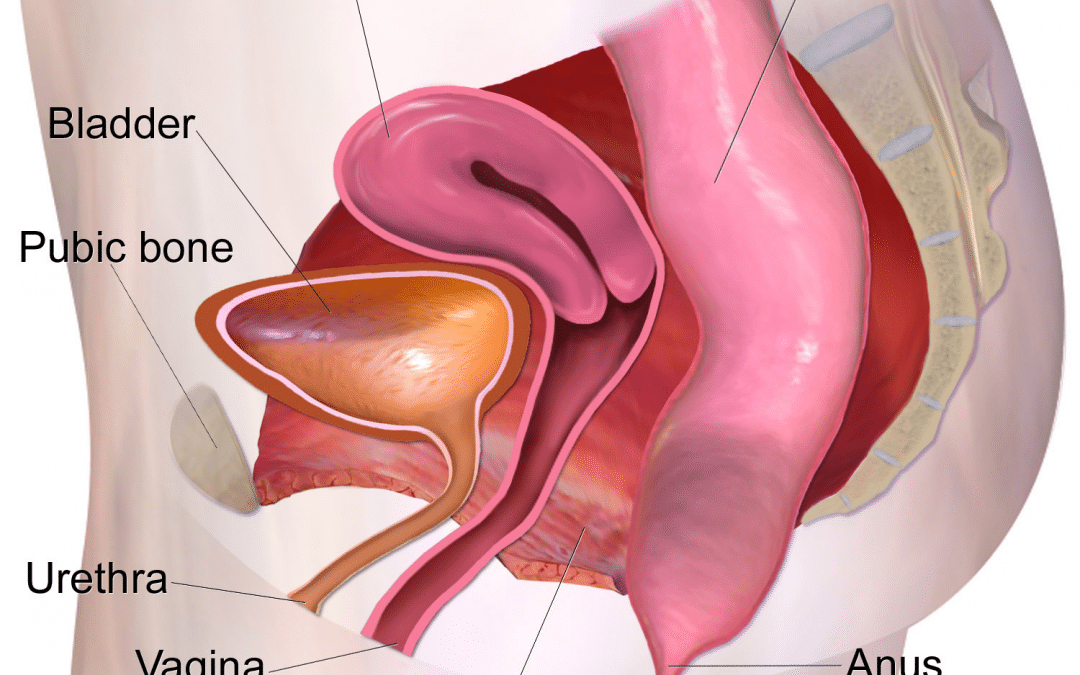
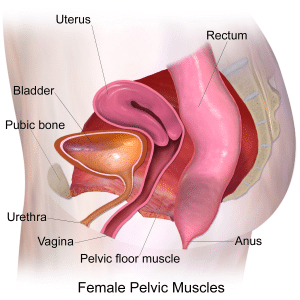
 The pelvic floor is the layer of muscles that stretch under the pelvis and support the inner organs (bowels, uterus, and bladder). I had never heard of the pelvic floor until I started learning about pregnancy and birth. Even though I was already suffering from and getting treated for a pelvic floor dysfunction long before I became pregnant, no one, not my OB or physical therapist, explained what the pelvic floor muscles did and how they could impact my well-being.
The pelvic floor is the layer of muscles that stretch under the pelvis and support the inner organs (bowels, uterus, and bladder). I had never heard of the pelvic floor until I started learning about pregnancy and birth. Even though I was already suffering from and getting treated for a pelvic floor dysfunction long before I became pregnant, no one, not my OB or physical therapist, explained what the pelvic floor muscles did and how they could impact my well-being.
Turns out, as I would later learn, my pelvic floor could wreak a lot of havoc on my body during pregnancy and labor. My pelvic instability lead to symphysis pubis disorder that caused excruciating pelvic girdle pain that still lingers today, one year after I gave birth. The pulling on my pelvic muscles also lead to a lot of back pain.
To learn more about pelvic health, I reached out to Rachel Parrotta, DPT, a pelvic health physical therapist.
During Birth
“I believe that all people would benefit from learning about their pelvic floor muscles prior to giving birth,” Dr. Parrotta said. “Since we are often unfamiliar with these muscles, it can be difficult for people to use their pelvic floor muscles in ways that help facilitate both birthing and post-partum recovery.”
Imagine, you are in labor and your care provider says, “Okay, it’s time to push.” Many birthing people may feel that bearing down feeling, that urgent need and desire to push. However, receiving an epidural can prevent people from experiencing bearing down and even from pushing effectively because the abdominal and pelvic floor muscles feel numb. Care providers do something called “coached” or “directed pushing” until the laboring person gets the hang of how to push. Your care provider will tell you when and how to push in accordance with your contractions.
This happened to me. I got an epidural during back labor and didn’t have the bear down feeling until my water broke. My midwife coached my pushing because I wasn’t using my pelvic floor muscles correctly. She told me I wasn’t doing right. She got frustrated and impatient with me. She actually shoved her finger up my bum WITHOUT INFORMED CONSENT to pinpoint the muscles I should be using – an action that still makes me shudder and feel small to this day. I don’t want this to happen to you.
Pushing Practice
Ideally, we want our pelvic floor muscles to be relaxed during the second stage of labor (pushing), as tensing those muscles can actually delay birth. You can go to a professional like Dr. Parrotta to identify your pelvic floor muscles and learn how to use them for pushing BEFORE labor.
“Learning about your pelvic floor muscles prior to birth can help prepare for a more effective pushing phase of birth, especially if a person is planning on birthing with an obstetrician and/or with an epidural,” said Dr. Parrotta.
Pushing your baby into the world is a powerful action that we are all capable of doing. Exploring your pelvic floor to ensure its health and learn about its abilities can make an impact on your birth and postpartum experiences.

 What are normal symptoms in pregnancy?
What are normal symptoms in pregnancy?
 What are normal symptoms in pregnancy?
What are normal symptoms in pregnancy?

 Folate is a naturally occurring form of B9, while folic acid is a synthetic form.
Folate is a naturally occurring form of B9, while folic acid is a synthetic form.
 My chiropractor,
My chiropractor, 
 So, it’s important to practice stress reduction techniques like mindfulness and self-care. That’s why I created my
So, it’s important to practice stress reduction techniques like mindfulness and self-care. That’s why I created my 
 What Do You Need to Eat for a Healthy Pregnancy?
What Do You Need to Eat for a Healthy Pregnancy?
 Constipation
Constipation


 At around four months postpartum, I received an invitation to the
At around four months postpartum, I received an invitation to the 

 The
The
Recent Comments